Digital Health Consumer Adoption: 2015
For full access to our consumer adoption reports and survey data, become a Rock Health partner—email partnerships@rockhealth.com.
Historically, the consumer space in digital health has been one of the most challenging categories for investors, including Rock Health. The failure to discover and build massive companies has led to fear, anchored to widely-held perceptions of the consumer relationship to healthcare.
In search of real data around the space, we surveyed thousands of individuals (representing the entire U.S. adult population). Our goal was to answer a few key questions: 1) What are the current rates of penetration for the major B2C digital health categories? 2) What are the primary demographic and attitudinal drivers of adoption? 3) What are individual’s attitudes towards data privacy and who do consumers trust in terms of sharing health data? This report presents the data from our most recent survey, run over the summer and including over 4,000 individuals.
The results may surprise you. Often-heard digital health memes, including that the only users in these categories are young, educated, rich, and healthy turn out to be false. Instead, our study found that an individual’s attitude towards healthcare (responsibility, self-management, and willingness to pay out-of-pocket) was a major indicator of adoption. We found the unhealthy are adopting faster than the healthy. And finally that digital health adoption closely mirrors general technology adoption (an unassailable trend across all demographics). However, given that penetration is still low (i.e., in the early adopter side) across many of the surveyed categories, we fully expect demographic gaps to open up, particularly around age and income.
The need for consumer engagement in healthcare has never been higher. And yet, nearly half of Americans have used only one or none of the major digital health categories. No iconic company exists in the consumer category, perhaps representing one of the largest opportunities in digital health. We’re excited to add some data to the conversation.
Survey overview
The Rock Health Digital Health Consumer Survey tested adoption of six major categories of digital health technologies and attitudes towards data privacy and sharing within the healthcare ecosystem.
Survey overview
- Rock Health conceived and wrote all questions and materials used in the survey
- The denominator for this survey is internet-connected U.S. adults; when stating adoption metrics as a percentage of the population, the report is referring only to internet-connected adults
- The survey was designed to be <15 minutes in length with three main sections: demographics, attitudes and preferences, and adoption trends
- The maximum number of questions a respondent could have answered was 101 questions; question formats ranged from multiple choice to Likert Scales to open responses
Demographics
- Basic demographic questions (e.g., age, income, education, household size, gender, race, employment, and zipcode)
- Health status (e.g., insurance coverage, self-reported state of health, # of prescription drugs, # of hospitalizations, # of chronic diseases, and # of doctor visits)
- Technology adoption (e.g., smartphone user, active app user, social media user)
Digital health adoption
- Adoption levels, recency of usage, and actionability for online health information across type of information
- Adoption levels, recency of usage, plans to use, actionability, and most helpful characteristics of online reviews of healthcare services
- Adoption levels and mediums of tracking health factors
- Adoption levels, recency of purchase, plans to purchase, reasoning for purchase of wearable devices, and channel through which device was received
- Adoption levels, recency of usage, plans to use, and satisfaction rates for genetic-based services
- Adoption levels, recency of usage, plans to use, and satisfaction rates for telemedicine services
Attitudes and preferences
- Agreement with data privacy and sharing scenarios (i.e., sharing health data in specific use cases)
- Willingness to share various health data with industry stakeholders for a range of health data types
- Level of trust and perceived alignment across stakeholders by rank
Adoption
The primary objective of our survey was to test the current penetration of six core digital health categories that operate within B2C market contexts.
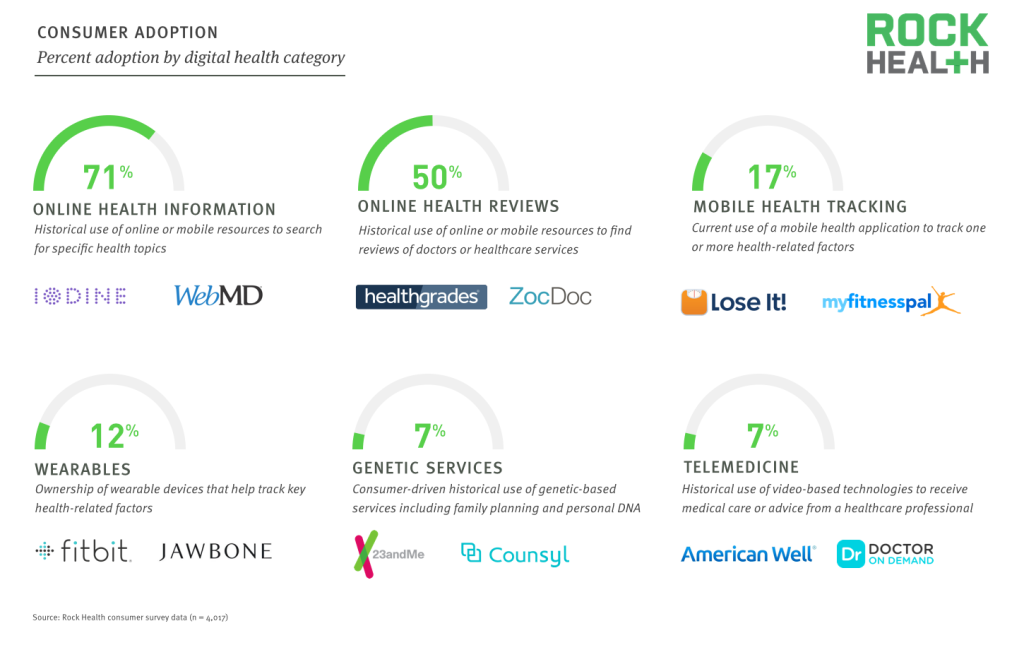
Source: Rock Health consumer survey data (n = 4,017)
There are a number of digital health companies (established and otherwise) working to redefine the way consumers interact with the healthcare system. These companies are attempting (or have attempted) to establish direct to consumer business models and fall into six overarching categories: online health information (e.g., WebMD), online health reviews (e.g., ZocDoc), mobile health tracking (e.g., MyFitnessPal), wearables (e.g., Fitbit), consumer-driven genetic services (e.g., 23andMe), and telemedicine (e.g., Doctor on Demand).
In healthcare, consumers have historically been one step removed from not just payment, but also decision-making. In spite of this separation, health remains innate to each individual, and there is a growing desire by the industry to make consumers responsible for payment, necessitating a change in how they understand and manage their own health.
These categories represent key parts of the consumer lifecycle in healthcare, from understanding their own conditions and finding a physician, to proactively tracking their health and disease, and finally accessing convenient care.
Digital health still faces a steep climb up the adoption curve, with nearly half of consumers having used only one digital health technology or having not adopted any at all.
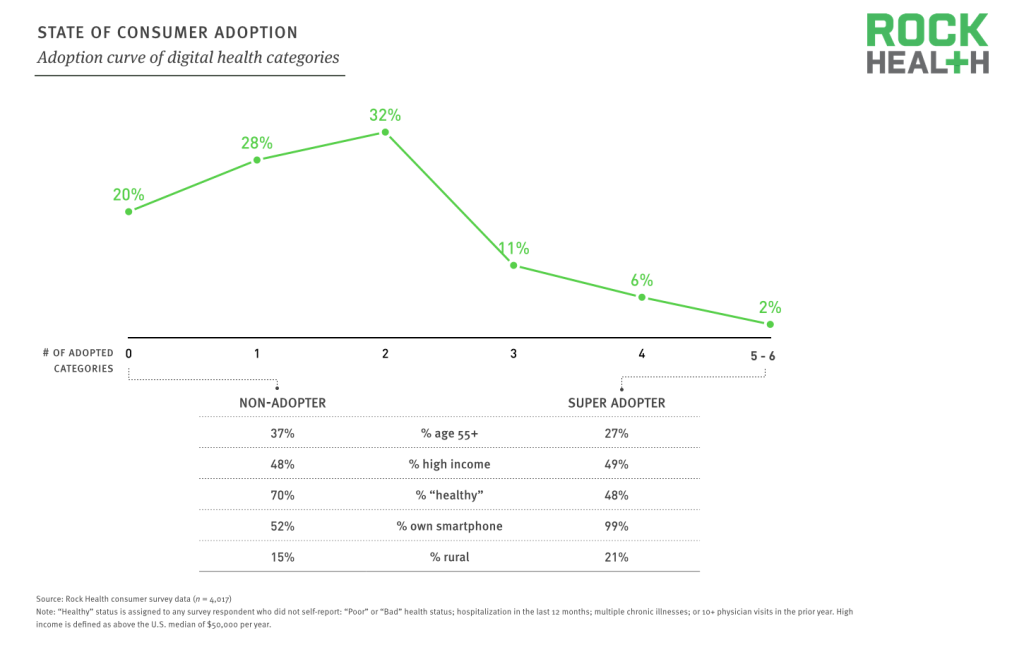
Source: Rock Health consumer survey data (n = 4,017)
Most Americans (80%) have used at least one of the digital health categories studied in this survey. Forty-eight percent have used zero (“non-adopters”) or exactly one of the technologies listed. On the other end of the spectrum, only 2% of people have used five or six of the technologies (“super adopters”).
There are key differences between these two types of individuals: non-adopters and super adopters. Super adopters tend to be younger, sicker, and significantly more likely to own a smartphone.
Searching online for health information is the most well-adopted digital health category, with 40% of those who search acting directly upon the information they find.
The survey looked at historical searching for specific health categories, including: diagnosis (based on symptoms), treatment options (based on a diagnosis), prescription drug information, and supplement information. Overall, 71% have previously searched online for these types of information, with six out of ten individuals searching for prescription drug information (the highest ranked category) and just under half searching for treatment options (the lowest).
Actionability of information was tested along a single dimension—whether it caused the person to present their findings to their physician, or in the case of supplements, to purchase or discontinue use. Across the board, about 40% of people who searched then chose this path of actionability, including a staggering 35% of those who search for a diagnosis proposing it to their physician, and 36% of those who search for treatment doing the same.
This group of consumers, representing approximately 15-20% of the U.S. adult population, is the highly activated base in our healthcare system—they are hungry for information, and confident enough to discuss it with their physicians (whether they are interested or not is a separate question).
While the adoption question focuses on searching for health information online, when asked to force rank the trustworthiness of health information sources, consumers ranked health websites, mobile health apps, and social media/online communities behind physicians and friends/family. Health information websites still need to do significant work to improve their general trustworthiness, beginning with adding minimal personalization and context for consumers.
Nearly half of Americans go online to find reviews of physicians, valuing customer comments and quality most when making a selection.
The survey assessed whether consumers had ever sought reviews across four separate categories (physicians, hospitals, nursing homes, and caregivers). Across all categories, approximately 50% of respondents sought online reviews, more than half of which (in aggregate) used the reviews to make selection decisions.
Those who had selected based upon reviews were asked to indicate which of seven characteristics (quality of care, customer comments, location, what insurance they accept, appointment availability, ease of scheduling, and price) had been most helpful in terms of making a decision. The answers indicate consumers are heavily leaning on the information they have been previously trained to seek in reviews: quality (think of the Amazon star rating) and customer comments (think of Amazon customer reviews). Price was a non-factor (likely due to unavailability of information), while the price proxy test of insurance accepted also did not score highly.
With the vast majority of Americans continuing to rely on informal caregiving, it’s no surprise that few are going online to look for reviews of formal caregiving. As the population continues to age, and children live further from their elderly parents, it’s likely many will start to augment and shift informal caregiving delivered personally to formal services. Accordingly, it’s inevitable that this generation will turn to digital services to find the best care.
There is a tremendous opportunity for solutions that include the informal caregivers who are taking care of the their loved ones and more likely to be an early adopter. Effective digital health solutions can help them deliver better care.
With the exception of physical activity, more consumers are currently tracking key health factors on paper or in their heads than with mobile applications.
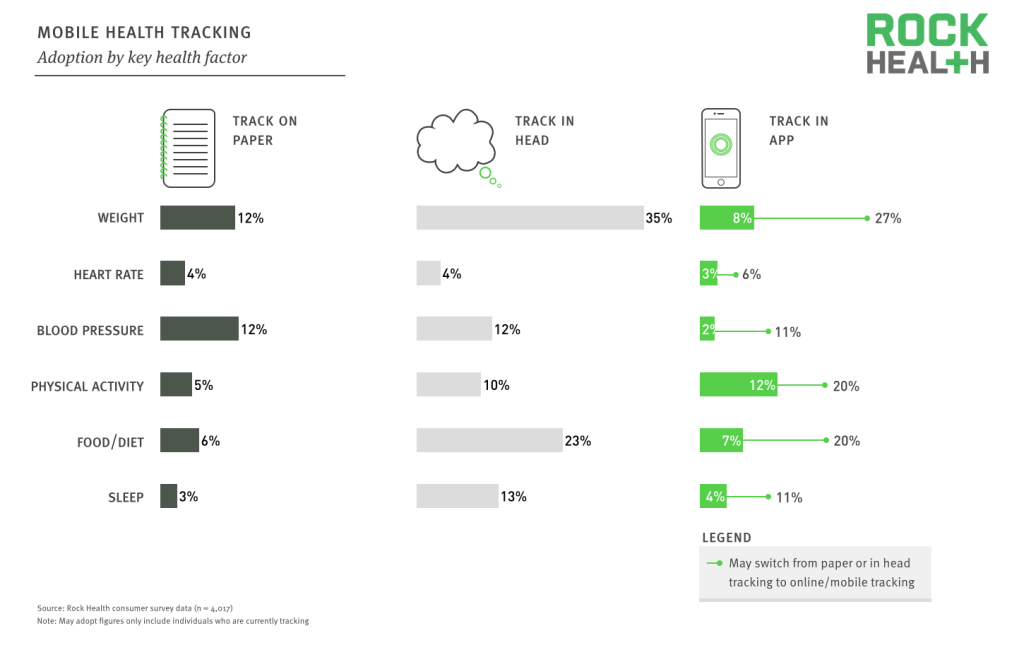
Source: Rock Health consumer survey data (n = 4,017)
Seventeen percent of the population is currently tracking a key health factor in a mobile application, suggesting that this category has begun to move beyond the “quantified self” movement. With significant parts of the population tracking multiple key health factors on paper or in their heads, it is not surprising to see some of this activity move towards mobile devices. It is obvious that the factors which currently dominate in paper tracking (weight and blood pressure) are the most likely to shift towards mobile-based tracking.
Physical activity was the sole health factor that more people tracked in a mobile app than on paper or in their heads. It is likely that passive monitoring has played a major role here, with motion sensors embedded in the vast majority of smartphones. Despite the lack of interest in heart rate tracking, we expect the proliferation of heart rate monitors on wristbands and smartwatches to push the percent tracking on mobile to grow quickly.
Consumers are most likely to buy wearable devices for themselves with the intention of becoming active and losing weight.
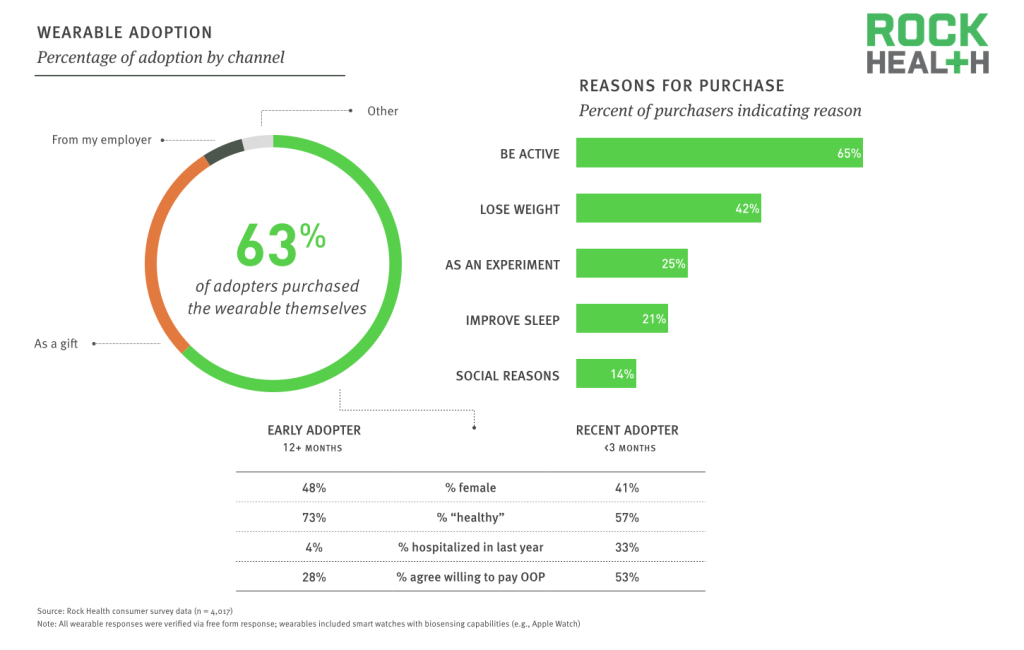
Source: Rock Health consumer survey data (n = 4,017)
Lifetime ownership of wearables reached 12% and three-quarters of owners reported received their wearable device in the last twelve months. Nearly two-thirds of individuals are purchasing wearables for themselves, with most citing the factors of being active or losing weight.
There are likely two major contributors to the attrition and rapid engagement decay rates noted in many other surveys. First, 28% of individuals are receiving wearables as a gift; and second, of those who purchase, 25% cite that they are doing so as an experiment. The implication of the second reason is that they do not set out with long-term ownership interest.
The demographics of wearable owners have begun to shift: recent purchasers are more likely to be unhealthy, including high rates of hospitalization, countering the popular narrative of only healthy individuals purchasing wearables.
While consumer-driven adoption of genetic services is relatively low, satisfaction is high and many consumers are considering using these services in the future.
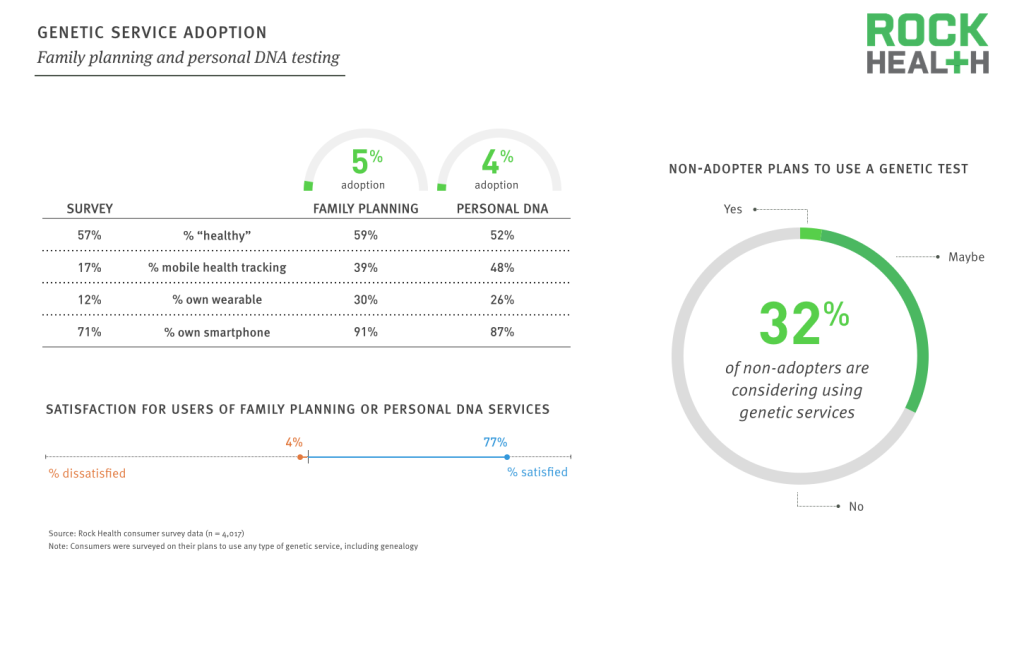
Source: Rock Health consumer survey data (n = 4,017)
Historical usage of consumer-driven genetic services (family planning and personal DNA tests) remains low at 7% between the two categories.
Adopters of these specific types of genetic services are significantly more likely to also engage in personal health tracking, including tracking of key health factors on their mobile phone and owning wearable devices.
More than two-thirds of non-adopters currently have no plans to use a genetic service, suggesting mainstream use cases beyond genealogy are still yet to be discovered.
Usage of telemedicine is highest amongst the 35-54 age bracket across all mediums, with adopters reporting high satisfaction.
Telemedicine (across email, text, and video channels) was the only individual digital health category that showed significant differences in adoption based upon age. Younger and older individuals tend to adopt at lower rates than middle-aged individuals, suggesting those who have had limited interaction with the healthcare system (the young) and generally lower technology penetration (the old) are less inclined to explore this new method of receiving healthcare services.
Telemedicine is an obvious hit with consumers, with those who use the channel highly satisfied overall. This suggests that the largest barrier to long-term replacement of many in-office visits is getting patients to their first virtual visit.
While video-based telemedicine is the least utilized medium today, nearly half of video-based telemedicine usage has occurred in the past 3 months, suggesting it is entering a rapid growth phase, particularly as consumers become more comfortable with video-based technologies (e.g., Facetime) generally.
Trust and education are really important factors when it comes to overcoming adoption barriers, since they address concerns such as ‘who are these doctors?’ and ‘what can they really do?’
Telephone is the preferred medium for telemedicine across both urgent and non-urgent use cases, although video ranks higher amongst those who have previously used it.
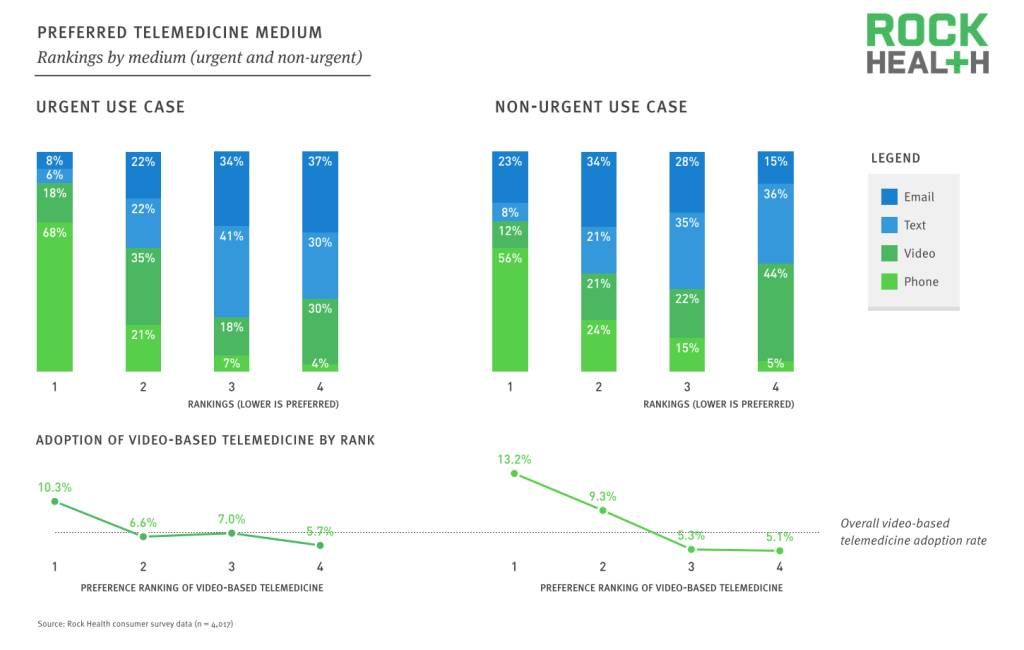
Source: Rock Health consumer survey data (n = 4,017)
When asked to force rank the various potential mediums for a telemedicine encounter, consumers overwhelmingly prefer phone (a non-digital medium) in both cases. Video is the second most-preferred option in an urgent situation, while email ranks second in non-urgent cases.
Preference for phone-based telemedicine, particularly in non-urgent use cases, appears to be an artifact of video being a nascent technology. Adoption rates for those individuals who show a preference for video are 2-2.5 times greater than those who ranked it non-preferable.
Wearables and telemedicine are set to be the fastest growing digital health markets in the near-term, with many also considering tracking health on their phone.
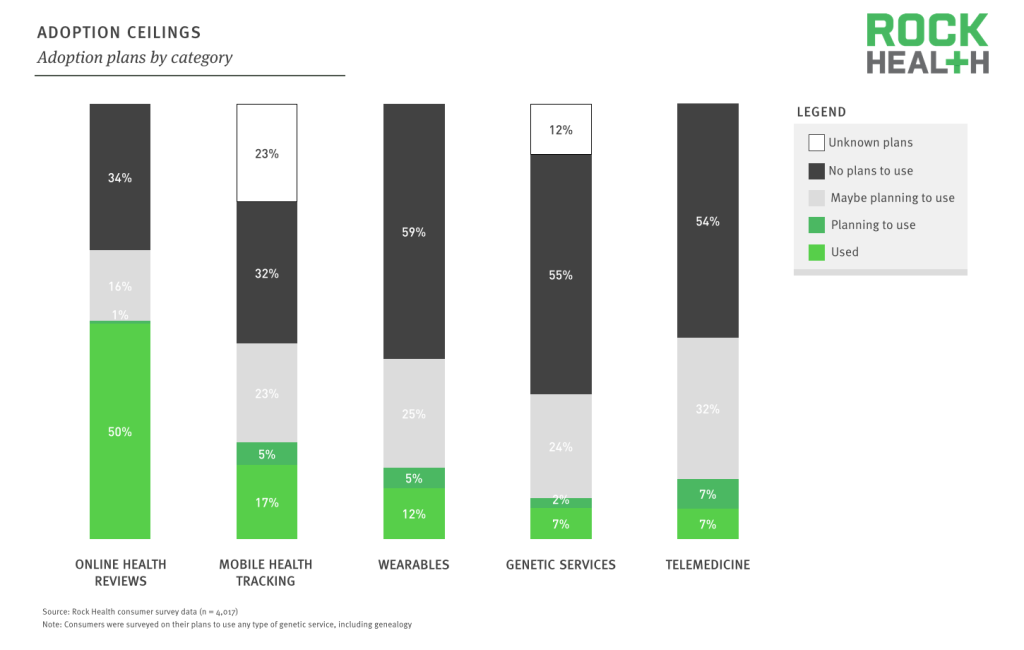
Source: Rock Health consumer survey data (n = 4,017)
When non-adopters were asked whether they planned to adopt digital health technologies, consumers responded most favorably to telemedicine (100% adoption growth) and wearables (40%) suggesting that these two categories are likely to grow the fastest over the coming twelve months.
Awareness of these technologies is surprisingly high across the board, and nearly all of the digital health categories are under-penetrated relative to the number of individuals who are considering using them. Online health reviews face the biggest challenge for growth, with the majority of the unaddressed market stating they have no plans to use a review service.
Historically, price and awareness have been the largest hurdles. Helix believes that consumer awareness of genetics is at an inflection point—hardly a week goes by without some mention of DNA in the media, often from a new discovery.
Drivers
While 52% of consumers strongly agree they are responsible for their own health, only 7% would say the same about their willingness to pay out-of-pocket for healthcare.
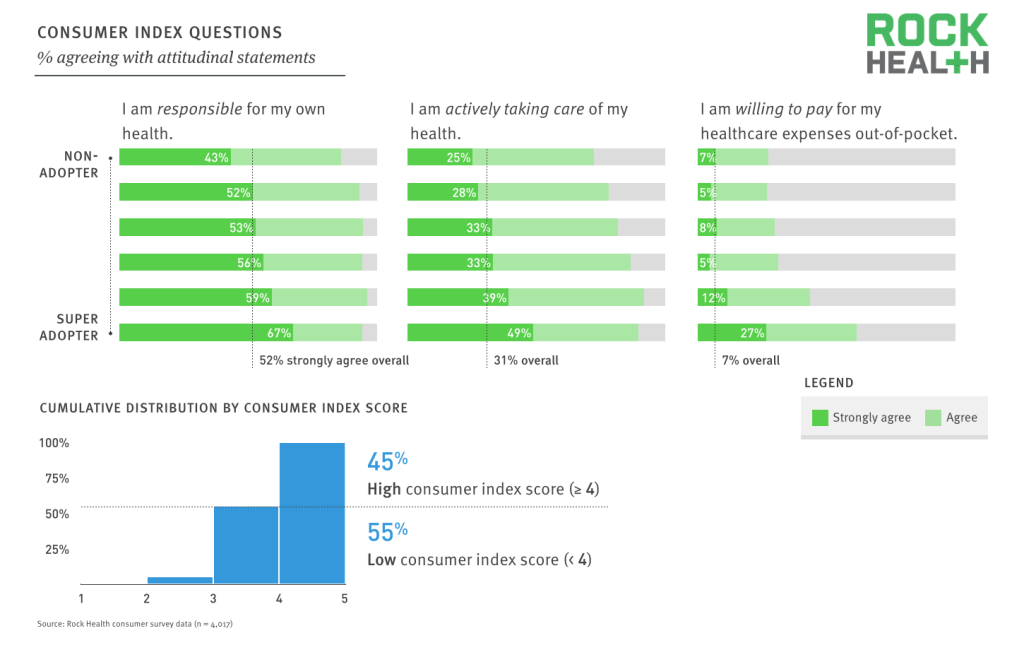
Source: Rock Health consumer survey data (n = 4,017)
While consumers generally feel responsible for their health and many are actively taking care of their health, less than 10% strongly agree with the concept of paying for health care expenses out-of-pocket, creating significant challenges for B2C businesses in digital health. Not surprisingly then, this set of attitudinal questions were highly correlated with the adoption of B2C digital health technologies.
Three attitudinal questions around how consumers perceive their relationship to healthcare were used to composite a “consumer index score.” 45% of respondents strongly agreed with at least two out of the three attitudinal questions and were considered to score “high” on the composite consumer index. All other respondents (55%) were classified as “low” on the index. The consumer index score was used to segment the population to better understand how consumer attitudes influence adoption.
The strongest indicators of adoption are health status and consumer attitudes, with unhealthy, highly consumer-oriented individuals adopting at the fastest rate.
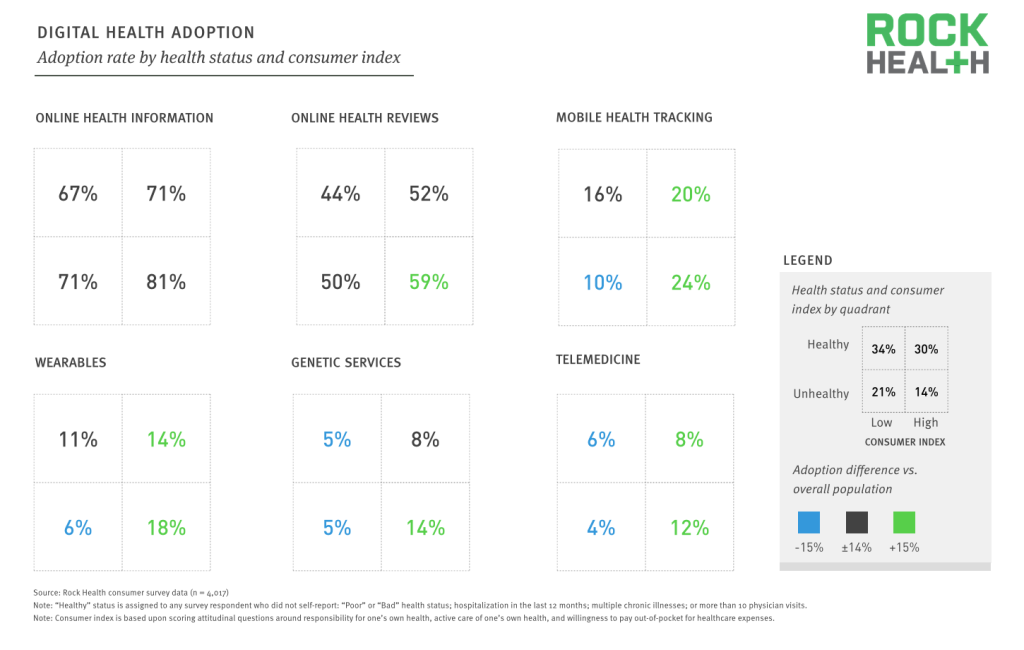
Source: Rock Health consumer survey data (n = 4,017)
Demographic variables including gender, age, income, and education were not found to have a statistically significant effect on adoption of digital health, except in a few specific cases. High income was a predictor of mobile health tracking adoption, and age/gender were both predictors of telemedicine adoption.
Consumer attitudes towards healthcare, specifically, how they scored on the attitudinal consumer index was found to have the most statistically significant relationship with digital health adoption. Broadly, those who are highly consumer-oriented consistently adopted at higher rates than those who scored low on the consumer index.
Adoption rates were reviewed at the intersection of self-reported health status and consumer orientation (high/low consumer index score). The largest segment of the population (healthy and low consumer index, 34%) are the slowest adopters of digital health, while the smallest segment (unhealthy and high consumer index, 14%) are the fastest adopters.
Note: “Healthy” status is assigned to any survey respondent who did not self-report any of the following: “Poor” or “Bad” health status; hospitalization in the last 12 months; multiple chronic illnesses; or 10+ physician visits in the last 12 months.
Privacy and data
While consumers vehemently agree they should be in control of health data access, the majority are willing to share data for personal and public health, along with discounts.
Consumers’ attitudes towards privacy demonstrate that there are not material concerns with sharing data under specific use cases, including for improved care (80% agree or strongly agree that they would share their health data for improved care), medical research (59%), and discounts on premium insurance (52%). Almost 40% of consumers indicated they would even be open to sharing their health data for money (no use case specified). However, they overwhelmingly (90%) agree or strongly agree that they should be in control of who has access to their health data.
This suggests that what is important to consumers is control and governance over their own data, not that they are unwilling to share. These attitudes reflect Apple’s health data strategy, which places control in the hands of consumers—they are responsible for provisioning access to specific data elements to specific apps (i.e., governing use cases) in the Health app.
When consumers are in control of their own data, they readily share it with health organizations. We see this daily and consistently, and it drives benefit to all healthcare stakeholders by increasing engagement and personalization of care.
Attitudes towards privacy and data sharing were found to be highly correlative with adoption of digital health technology. Answers to the four attitudinal questions (sharing for improved care, research, premium discounts, and money) were used to index a privacy score for each respondent. Individuals who scored in the upper two quintiles (i.e., top 40%) were significantly more likely to adopt multiple digital health technologies.
Physicians remain at the center of data in the context of healthcare, with consumers more willing to share their information with them than anyone else.
Consumers have a high willingness to share their health data, including health history, physical activity, and genetics, with the industry ecosystem, particularly with physicians.
It’s likely that insurance companies have underexploited their position in the market—consumers rank insurers second when it comes to being most aligned with their personal health interests and are generally willing to share activity data (48% willing to share) and health history (41%), although they are less willing to share genetic data (25%).
Absent physicians, sharing propensity drops by over a third across all health data types. Health history falls to a meager 56% willing to share, physical activity to 63% and willingness to share genetic data drops below 50%.
Only 18% are willing to share health data with technology companies, who rank above only the government in terms of alignment with personal health interests. Of tech companies, individuals are about half as likely to share their data with Facebook as they are with Google.
Methodology
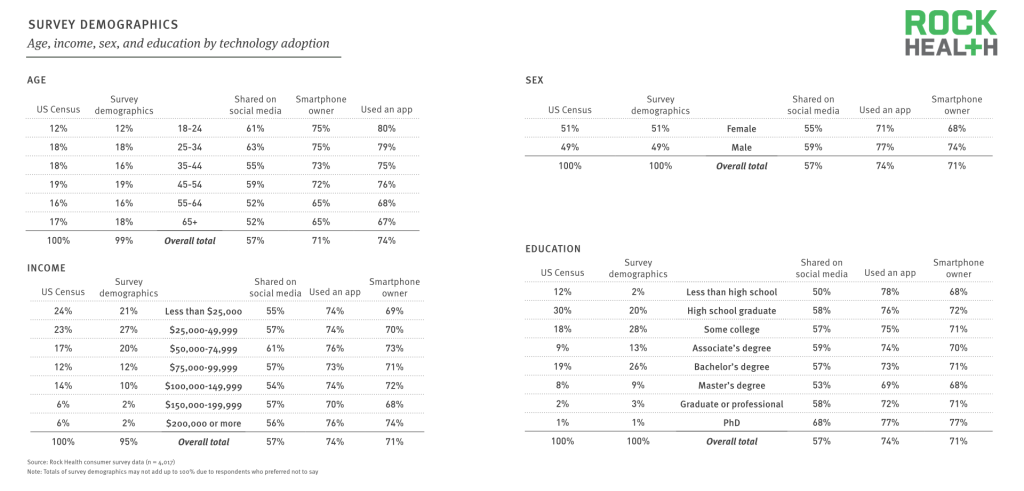
Source: Rock Health consumer survey data (n = 4,017)
Survey demographics
- Qualifying population: Incidence rate of 90%. Individuals with personal internet access, either at home, work or via their mobile phones were eligible to take the survey. Additional screening was based on demographic requirements.
- Demographic breakdown: With a sample size of n=4,017, respondents were a nationally representative population based on U.S. Census percentages for sex, age, and region. Soft quotas were met for household income and ethnicity.
- Survey timing: The full launch of the survey began on July 7, 2015 and ended on August 28, 2015.
Data quality
- Respondent quality: We employed Toluna to deploy our survey. To ensure data quality, Toluna authenticates all respondents and further validates against third-party data sources including the U.S. Postal Service and telephone directories. Additionally, flash/cookie-based and digital fingerprinting technologies were used to ensure there are no duplicate respondents. Industry standards for screening bad completes were used such as red herring questions and monitoring time for speeders.
- Response quality: For questions surrounding mobile health tracking, wearable devices, genetic services, and telemedicine, free response qualifying questions were used to validate whether a respondent had truly adopted the technology. All free responses were reviewed and coded by Rock Health—respondents with invalid answers were not included in overall adoption metrics.
Survey design and analysis
- Survey design: Rock Health conceived and wrote all questions and materials used in this survey. To ensure best practice survey techniques were used, Rock Health employed Toluna’s internal questionnaire review team.
- Survey analysis: Findings from the data were based on internal analyses conducted in R.
Watch the archived webinar to hear more insights from leading entrepreneurs in the B2C market.

