Welcome Collective Health
Each fall, tens of millions of people are subjected to the annual ritual of open enrollment. This staple of employer-sponsored health insurance (ESHI)—itself an artifact of a war-time wage freeze in the 1940s—has become a painful process, wrought with uncertainty and fear of making the wrong choice.
The yearly decision around health benefits—determining how much we each pay for our healthcare and what access we are afforded to physicians, hospitals, and treatments—has a significant impact on a company and its employees. It’s a process that begins long before open enrollment, with a sea of service providers spanning health insurers, analytics vendors, and consultants advising companies on forecasted spend and the optimal plan designs.
These choices end up directing over $900B in health expenditures each year. And yet the decisions are largely outsourced—companies have a limited set of tools to drive decision-making, relying solely on black box wielding actuarial consultants delivering an annual insight. Lacking the information and resources, the market has also split between large companies that are able to enjoy the cost savings of insuring themselves (the self-insured) and smaller companies that rely solely on health insurers (the fully-insured) and that are further subject to costly mandates, significant year-to-year premium fluctuations, and heightened regulatory requirements.
Enter Collective Health.
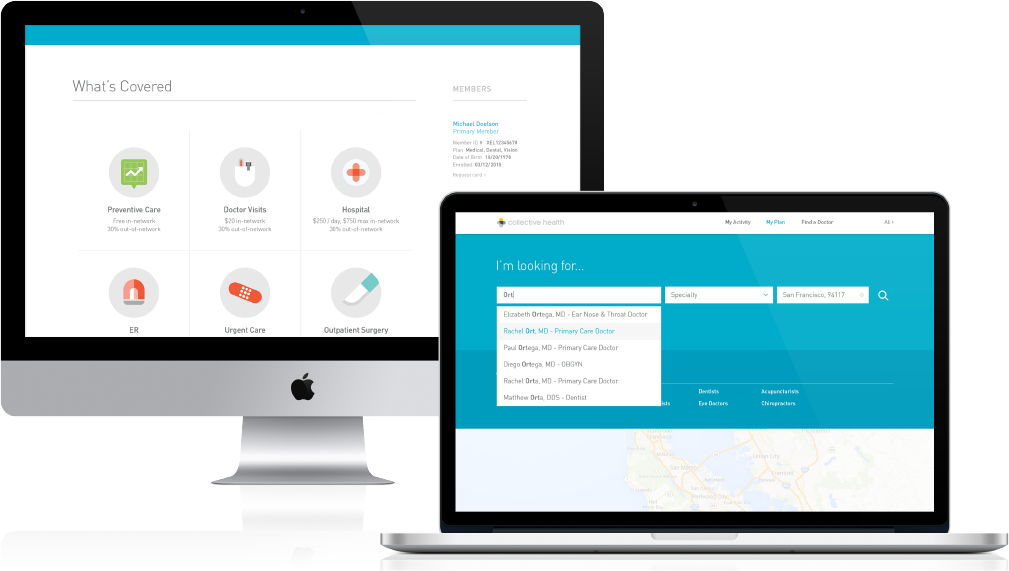
Collective Health is bringing a modern SaaS platform to employer-sponsored health insurance (ESHI). It helps small companies convert from being fully-insured to self-insured, and provides all of the tools (including forecasting) necessary to manage their own benefits. The platform can also be used by any company that is self-insured today, offering complete flexibility around plan design and management.
The SaaS platform seamlessly integrates with existing HR and finance systems, and because Collective Health is a third-party administrator (claims processor), it is able to wrap the entire employer experience in real-time analytics. This allows talent managers to make informed decisions throughout the year on health benefits and programs. Collective Health marries this world-class employer engine for health benefits management with a thoroughly redesigned employee experience. They’ve cut the jargon out of health insurance, allowing users to readily understand their benefits and costs.
The infrastructure of ESHI is critical—the vast majority of Americans receive their health insurance through employers (nearly 170M in total), and despite the success of Health Insurance Exchanges, the employer-based market isn’t going anywhere. Collective Health is building an entirely new benefits experience for both employers and employees at the foundational level. Success here will underpin a dramatic modernization of ESHI, creating a vast opportunity not only for Collective Health, but the many other startups that attempt to partner with health insurers or penetrate employers. Larger vision aside, I’m confident that this year’s open enrollment will at minimum be less painful for Collective’s customers.
We are thrilled to be investors in Collective Health and welcome Ali, Rajaie, Kent, Preston, and the entire Collective Health team to our burgeoning community of entrepreneurs. If you want to join an outstanding team focused on transforming one of the most important markets in healthcare, you should check out the open positions at Collective Health.